Treatment for gum recession varies with cause and severity; you will learn how aggressive brushing, periodontal disease, tobacco, and genetics contribute, what non-surgical and surgical options (scaling and root planing, soft-tissue grafts, guided tissue regeneration) can restore health, and practical prevention strategies you can apply to protect your gums and preserve your teeth.
Understanding Gum Recession
When your gingival margin migrates apically and exposes root surfaces, you face increased sensitivity, root caries, and aesthetic changes. Recession may be localized or generalized, progress over months to years, and commonly links to periodontal infection, aggressive brushing, tooth position or orthodontic movement, and tobacco use.
What is Gum Recession?
Gum recession is the apical displacement of the gingival margin that uncovers cementum and root dentin; those tissues are less mineralized than enamel and demineralize faster. You may see increased pocket depths or exposed root surfaces that stain, and loss of attachment is measured in millimeters with a periodontal probe.
Common Symptoms and Indicators
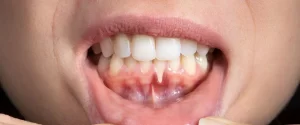
You’ll often notice longer-looking teeth, notches at the gumline, and sensitivity to cold or sweets; bleeding on probing and higher plaque retention are frequent signs. Even 1-2 mm of root exposure can produce sensitivity, while defects beyond 3 mm significantly raise the risk of root caries and mobility.
Clinically, recession patterns vary: a single Miller Class I defect on a canine differs from generalized marginal tissue loss across molars. If you present with asymmetric recession, assess occlusion, brushing technique, and prior periodontal therapy; for multiple sites, evaluate systemic factors like smoking or diabetes and record recession depth, probing depths, and gingival phenotype in your chart.
Causes of Gum Recession
Gum recession results from a mix of biological and behavioral causes: periodontitis that destroys attachment, mechanical trauma from aggressive brushing or ill-fitting restorations, tooth positioning that places roots thinly beneath bone, and long-term habits like smoking or mouth breathing. You may also see recession follow orthodontic movement when roots move outside the alveolar plate. Often several factors act together, so evaluating your hygiene, bite, and lifestyle helps pinpoint drivers of your recession.
Genetics and Heredity
Your genetic profile influences gingival thickness and attachment: a thin periodontal biotype makes you far more likely to exhibit recession with even mild insults. Families often show similar patterns-if relatives developed early recession, suspect hereditary susceptibility. In practice, thin tissue around canines and premolars tends to recede first, so you may need tailored prevention or grafting strategies to protect roots long-term.
Environmental Factors and Habits
Environmental contributors include tobacco use, abrasive brushing, bruxism, oral piercings, chronic mouth breathing, and acidic diets that weaken soft tissue and enamel. You commonly find localized recession where a habit concentrates force or irritation-such as a barbell rubbing the gingiva or a quid tucked under a molar. These behaviors both accelerate tissue loss and reduce the success of healing after treatment.
- Smoking and smokeless tobacco constrict blood flow and impair healing
- Aggressive horizontal scrubbing with hard bristles abrades the gingival margin
- Bruxism and clenching create focal trauma on facial root surfaces
- Oral piercings physically rub and ulcerate adjacent gum tissue
- This cluster of habits markedly increases your risk of progressive recession
If you grind, recession typically appears on facial surfaces of lower incisors and premolars within months to years unless you use a night guard; correcting bruxism often stabilizes the condition. If you use tobacco or a tobacco quid, expect slower tissue healing and deeper pockets after therapy. With oral piercings, recession can begin at the contact point and progress despite good hygiene, so habit modification determines long-term treatment success.
- Stop tobacco and maintain regular professional periodontal maintenance
- Switch to a soft-bristle brush, use gentle vertical strokes, and refine technique
- Wear a night guard for bruxism and consult about occlusal correction
- Remove or reposition oral jewelry that contacts your gums
- This set of habit changes significantly lowers the chance of further recession
Treatment Options for Gum Recession
You can choose treatments based on recession severity and symptoms: mild cases often respond to non-surgical care while deeper defects typically need surgery. Scaling and root planing with improved home care reduces inflammation and pocket depth by about 1-2 mm on average, desensitizing varnishes cut sensitivity for many patients, and restorative composites can mask defects in a single visit. Surgical grafting can restore tissue with reported mean root coverage of roughly 70-90% for well-selected defects.
Non-Surgical Treatments
Your first-line options include scaling and root planing, topical fluoride or potassium nitrate for sensitivity, and composite bonding to cover exposed roots. Orthodontic repositioning or occlusal adjustment may reduce further recession in specific cases, and night guards protect against bruxism-related trauma. Conservative measures often stabilize recession in mild-to-moderate cases within 3-6 months when combined with strict plaque control and regular professional maintenance.
Surgical Treatments
Your dentist or periodontist may recommend connective tissue grafts, free gingival grafts, coronally advanced flaps, or guided tissue regeneration for more advanced recession. Connective tissue grafts paired with a coronally advanced flap are among the most predictable, with many reports showing mean root coverage of about 70-90% at 6-12 months. Expect initial healing in 1-2 weeks and tissue maturation over 6-12 months, with postoperative care including chlorhexidine rinses and short-term analgesics.
More specifically, connective tissue grafts commonly harvest 1-1.5 mm of palatal tissue and are sutured under a coronally advanced flap; alternatively, acellular dermal matrix allografts avoid a donor site and work well when palatal tissue is limited. Sutures are usually removed at 7-14 days, and success depends on blood supply, flap tension, and meticulous plaque control-studies show site selection and technique strongly influence final root coverage percentages.
Prevention Strategies
Oral Hygiene Best Practices
Brush gently for two minutes twice a day with a soft‑bristled brush held at a 45° angle and floss once daily; consistent interdental cleaning reduces plaque-related recession. Replace your brush every three months or when bristles splay, use fluoride toothpaste, and consider desensitizing paste (e.g., 5% potassium nitrate) for sensitivity. Schedule professional cleanings every 3-6 months based on risk and ask your hygienist about targeted scaling around recession sites.
Lifestyle Changes
Stop smoking-tobacco roughly doubles your risk of periodontal disease and impairs healing-manage bruxism with a night guard, and limit acidic drinks like soda and citrus that erode tissue and enamel. Control blood sugar (discuss HbA1c targets with your clinician) since diabetes accelerates gum breakdown, and reduce stress and poor sleep, which heighten inflammation linked to progression.
Use combined smoking-cessation strategies (counseling plus nicotine replacement or prescription therapy) to maximize success, and get a custom occlusal guard if you grind. Wait 30-60 minutes after acidic meals before brushing to avoid abrasion of softened surfaces, treat GERD if present, and coordinate diabetes care (often aiming for A1c <7% when appropriate) to lower periodontal risk.
The Role of Professional Dental Care
Professional care ties together home prevention and clinical intervention: your dentist and hygienist measure recession in millimeters from the CEJ, assess pocket depths, and decide when to escalate care. You benefit from scaling, root planing, and targeted maintenance intervals (typically every 3-6 months). When recession exceeds about 3 mm with root sensitivity or aesthetic concern, referrals for periodontal surgery or connective tissue grafts are common to restore tissue and prevent further attachment loss.
Regular Check-ups and Cleanings
Schedule check-ups every 3-6 months based on your risk profile so clinicians can remove calculus that brushing misses and monitor changes in pocket depth and recession in millimeters. Hygienists use ultrasonic and hand scaling, polish, and apply fluoride varnish when indicated. Studies show consistent periodontal maintenance markedly lowers the chance of progressive attachment loss and reduces long-term tooth loss, especially for patients with prior periodontal disease.
Potential Diagnostic Tools
Periodontal charting with a calibrated probe records probing depths, recession, and bleeding on probing in mm, while bitewing and periapical radiographs detect horizontal bone loss. You’ll also have mobility and furcation assessments to stage disease. These basic diagnostics guide whether non-surgical therapy suffices or whether advanced imaging and specialty referral are needed for definitive treatment planning.
Advanced tools include cone‑beam CT for 3D assessment of buccal bone defects and root morphology, intraoral cameras for photographic documentation of recession progression, and molecular microbial testing (PCR/DNA probes) to identify pathogens like P. gingivalis when considering adjunctive antimicrobials. Using digital radiography and serial probe measurements helps you and your clinician track response to therapy and tailor maintenance frequency and surgical planning accordingly.
Frequently Asked Questions
You probably want concise answers: about 50% of adults over 30 show some gum recession, and causes range from periodontitis to toothbrush abrasion and orthodontic movement. You can often halt progression with improved hygiene and periodontal therapy; desensitizing agents may relieve symptoms in 1-3 months, while surgical grafts typically require 6-12 months for full healing and measurable root coverage.
Common Concerns About Gum Recession
You often worry about sensitivity, root decay, and appearance; exposed roots increase sensitivity and susceptibility to root caries, and many patients ask about durability. Soft‑tissue grafts commonly provide 70-95% root coverage depending on the defect, while non‑surgical care and behavior changes can stabilize mild recession. Costs range from a few hundred to several thousand dollars, and long‑term success depends on controlling periodontal disease and avoiding further trauma.
Myths and Misconceptions
You may hear that aggressive brushing is the only cause or that gums will simply grow back on their own; neither is universally true. Genetics, inflammation from periodontitis, orthodontic forces, and occlusal trauma also drive recession, and spontaneous regrowth is rare-surgical grafts are usually required for significant coverage, with outcomes varying by technique and defect size.
If you want a practical example, consider a typical case: a 45‑year‑old with localized recession from a history of untreated periodontitis who switched to a soft‑bristle brush and received scaling and root planing-progression halted in about three months, and a connective tissue graft at six months achieved roughly 85% root coverage and resolved sensitivity by nine months, illustrating combined therapy and technique change yields the best results.
FAQ
Q: What commonly causes gum recession?
A: Gum recession occurs when the gum tissue pulls away from the tooth, exposing the root surface. Common causes include periodontal (gum) disease, aggressive or incorrect brushing, tobacco use, genetic susceptibility, tooth clenching or grinding, misaligned teeth, orthodontic movement, and oral piercings. Age-related tissue thinning and inflammatory responses to plaque also contribute. Identifying the underlying cause guides appropriate treatment.
Q: How is gum recession diagnosed?
A: Diagnosis involves a clinical periodontal exam with measurement of recession and probing depths, assessment of attachment loss, evaluation of tooth mobility and occlusion, and dental X-rays to check bone levels. Dentists may take intraoral photos and charting to monitor progression. A full medical and dental history helps link systemic factors (e.g., smoking, diabetes) or habits to the condition.
Q: What non-surgical treatment options are available?
A: Non-surgical care focuses on controlling inflammation and halting progression: professional scaling and root planing to remove plaque and tartar, improved oral hygiene with gentler brushing technique and a soft-bristled brush, targeted antimicrobial therapy when indicated, desensitizing agents or fluoride varnishes for sensitivity, occlusal adjustments or bite guards for bruxism, and behavioral changes like quitting tobacco. Composite bonding can cover exposed roots when surgery is not chosen.
Q: When is surgery recommended and what procedures are used?
A: Surgery is recommended for advanced recession with root exposure, aesthetic concerns, root sensitivity unresponsive to conservative care, or inadequate attached gingiva. Common procedures include connective tissue grafts and free gingival grafts to increase tissue thickness and cover roots, coronally advanced flaps to reposition gum tissue, guided tissue regeneration to promote attachment, and minimally invasive/laser-assisted techniques in select cases. The choice depends on recession depth, tissue quality, and patient goals.
Q: How can gum recession be prevented?
A: Preventive measures include maintaining regular dental checkups and professional cleanings, using a soft-bristled brush with proper light-pressure brushing technique, daily flossing, managing periodontal disease early, treating bruxism with a night guard, correcting malocclusion or harmful oral habits, avoiding tobacco, and protecting teeth during sports. Early intervention on gum inflammation and habit modification significantly reduce future recession risk.

